This is the first article of a two-part series written by our guest author, Matthew Papaconstantinou. The second article will be published on this blog in a few days time. You can read a bit more about Matthew at the end of this article.
The obesity epidemic captivating the modern world has caused morbidity and mortality rates to increase astronomically in the US, and abroad. Obesity is defined by a body mass index (BMI) score in the range of 30 or above. Due to its prevalence, it is now linked to a multitude of musculoskeletal problems causing debilitating joint pain and motion disability, including osteoarthritis (OA).
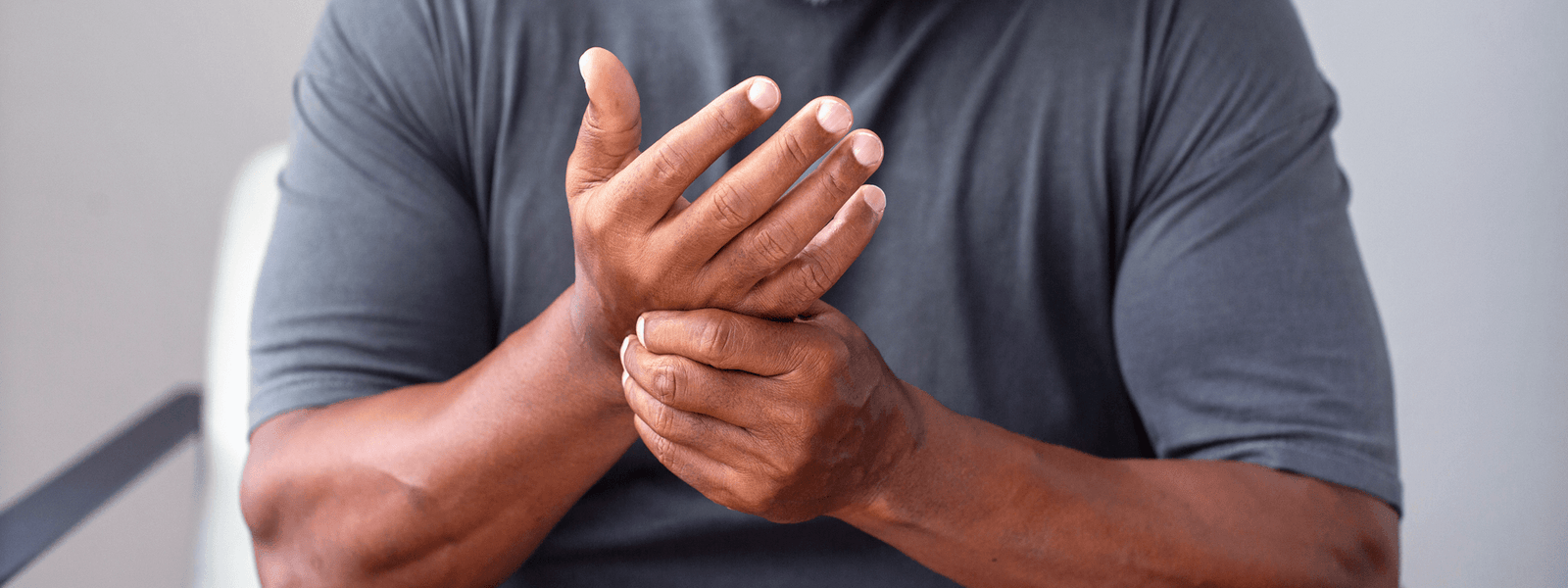
OA is a degenerative joint disease that involves the locking of joints, stiffness, creaking, and recurring inflammation. Concentrated primarily in the hips, knees, and hands—joint pain is the most common symptom of OA. Typically resulting from a loss of articular cartilage, the pain originally occurs only when the joint is used, before becoming increasingly constant in the latter stages.
Today, OA affects 27 million Americans and is the leading cause of disability in the US. It has now become the most prevalent joint disorder in the world, predominantly affecting the obese, aging population, attacking at least 70% of people over 65 years of age. Inevitably, OA exacts a heavy economic burden, accounting for 25% of primary care visits and at least 50% of all NSAID (Non-Steroidal Anti-Inflammatory Drugs) prescriptions, such as Orudis, Advil, or Aleve.
Most OA sufferers can find temporary relief using medication, acupuncture, and/or making dietary and lifestyle changes. However, many of the most common medications recommended have side effects that can cause severe reactions or even pose serious health hazards. Surgery tends to be the option considered most among those whose symptoms are so severe they find no reprieve. Hospitalizations for OA symptoms have increased 2.5 times since 1993.
Recent studies indicate that natural pain relief remedies are becoming increasingly effective. An example is the Glucosamine/Chondroitin Arthritis Intervention Trial (GAIT) whose results appear very promising. Today, there are at least 5 million people in the US supplementing their diets with glucosamine or chondroitin sulphate. The most advanced natural formula on the market today, Arthrit-Eze, is an example of a natural pain relief supplement containing these ingredients.
Is Obesity a Risk Factor for Osteoarthritis?
Many population-based studies have shown that obese individuals have an increased risk of developing OA symptomology. In an Australian population survey, conducted in 2001, the results of 7500 respondents indicated that the incidence of arthritis among the obese is twice as high, as compared to individuals with a BMI in the normal range (18.5 to 24.9), regardless of age and/or socioeconomic status [1].
Overweight and Knee OA
Results of many of the most current studies indicate a positive correlation between obesity and knee OA. In a study conducted among participants in the US, it was revealed that incidences of knee OA doubled for every five-unit BMI score increase. A Scottish survey revealed that the frequency of hip and knee pain among 858 respondents, an average age of 58, was twice as high, among obese individuals.
Over time, bony projections can form along the deteriorating joints damaged by arthritis. Scientifically, they are referred to as osteophytes, or bone spurs. One study showed that the risk of developing these bone spurs among overweight women with a BMI in the range of 25 to 29.9 was also twice as high as those in the normal range [2].
Likewise, compared to healthy individuals of the same age and gender, many of the joint replacement therapy candidates have also been identified as overweight or obese [3]. This data further confirms the trend between obesity and the incidence of lower limb joint pain, namely OA.
Overweight and Hip OA
Although incidences of hip OA are not as prevalent as those with knee OA, studies show that hip replacement surgical procedures (HRSP) are more common among individuals with early-onset obesity.
An example of this is found in data collected from the USA Nurses study, which indicated that an elevated BMI, at age 18, contributed to a five-fold increased risk of HRSP needed later in life [4]. A cohort study conducted in Norway of 1.2 million identified a risk 3.4 times greater of developing hip OA among the obese than those within the normal BMI range.
Overweight and Hand OA
Ironically, hands are not weight-bearing joints, however, people who are overweight and obese struggle with much higher incidences of hand OA. The findings of a 23-year study confirm this association between obesity and hand OA. Yet, their results insight more questions than provide answers, as to the hand OA origination. If OA in the knee and hip has a mechanist basis (placement of excessive force on the joints), then how can OA in the hand, a non-load-bearing joint, be explained?
Obesity and OA – Which Comes First?
The studies mentioned above show clearly that there is an association between incidences of obesity and OA. However, the issue of causation continues to arise. Researchers are trying to identify whether having OA leads to obesity or whether being obese leads to OA? In other words, someone may argue that the people who were overweight in these co-relational studies gained weight as a result of the limited mobility imposed by their arthritis condition.
This type of question can be answered only by a longitudinal study, a study that involves repeated observations over long periods. That was exactly the goal of the Framingham Heart Study. Among 1420 healthy participants, those who were found to be heavier, but OA-free, in their 30s, were also found to have an increased risk for developing OA in their 70s. This confirms that the prolonged presence of obesity is, in fact, a causal factor for OA.
Conclusion
Research has shown that individuals who are overweight or obese have an increased risk of developing arthritis, in addition to a multitude of other chronic diseases (e.g. heart disease, diabetes, osteoporosis, cancer, etc.). More specifically, obesity can be directly attributed to higher incidences of knee OA and is related to the development of hip and hand OA, as well. Ultimately, weight management, in addition to proper supplementation, is one of the most effective treatments for those diagnosed and living with the debilitating effects of OA.
About the Author
Matthew Papaconstantinou, PhD, is a biology researcher, with a great interest in the relationship between obesity and diseases of the joint. Matthew analyzes current trends in diets and weight loss programs and makes a promotional code for BistroMD diet and coupon codes for Diet To Go, two doctor-endorsed meal replacement plans, available through his blog.
References:
- Role of age, sex, and obesity in the higher prevalence of arthritis among lower socioeconomic groups: a population-based survey. Busija L, et al. The University of Melbourne, Melbourne, Victoria, Australia.
- Incidence and risk factors for radiographic knee osteoarthritis in middle-aged women: the Chingford Study. Hart DJ, Doyle DV, Spector TD. Arthritis Rheum. 1999 Jan;42(1):17-24.
- Coggon D, Reading I, Croft P, McLaren M, Barrett D, Cooper C. Knee osteoarthritis and obesity. Int J Obes Relat Metab Disord 2001;25:622–7
- Felson DT, Anderson JJ, Naimark A, Walker AM, Meenan RF. Obesity and knee osteoarthritis. The Framingham Study. Ann Intern Med 1988;109:18–24


 Supplements
Supplements Bundles
Bundles